Is it Addiction? Or Just a Bad Habit?
Note: Nothing in this article is intended to diagnose or treat a mental or physical health condition. If you are concerned that you are dealing with any kind of psychological or physical dependence on a substance or behavior, please reach out to a qualified medical and/or mental health professional for support. The same is true if you are dealing with any kind ofhormonal and/or nutritional issues. If you are experiencing a crisis, please reach out to your local emergency services or a local crisis line.
Once You See It…
When I first started dealing with some hormonal issues, I had no idea that trying to follow some basic nutrition guidance would illustrate up-close and personal the true difference between a habit and an addiction.
The instruction was straightforward enough: manage glucose spikes by eating fewer refined carbs and reduce extra sugar. I knew it was going to be rough as food has always been a source of comfort, but I jumped right in. With my health on the line, making these changes was a major priority.
What followed gave me far more insight into my own behaviors than I had expected. I could slow down with the white bread without much fuss, but the sugar was a different story.
While it took me a minute to admit it, in retrospect it was clear as day. The white bread was a habit. And the sugar? An addiction.
And once you see it… you can’t unsee it.
Why is it so Hard to Tell The Difference?
The short answer is that addictions and “bad” habits can look almost identical.
At their core, they both involve resorting to repeated, automatic behaviors to meet an underlying need or desire in the short-run, but that also have negative consequences. We also usually have some degree of resistance to making changes around these behaviors while simultaneously judging ourselves for engaging in them (or we wouldn’t call it a “bad” habit).
What makes it even harder to tell a habit from an addiction is that the exact same behavior can be either one, including:
Substance use
Gambling
Exercise
Dating/romantic relationships
Shopping/overspending
Food (sugar, fast food, etc.)
Pornography
Social media (including all short-form video platforms)
Video games/mobile games
Work
Sex
Screens
Some behaviors less typically thought of in this context include:
Control
Procrastination
Perfectionism
Information/knowledge (including the news)
Socializing patterns (withdrawing or hypersocializing)
Eating patterns related to bingeing, dieting, and/or restricting food (including “clean” eating)
Self-help/spirituality (including books, retreats, therapy/coaching, peak/transcendent experiences)
Note: These things only become “bad” habits or addictions when we are using them to bypass or override our difficult internal experiences rather than to truly recover, heal, or connect with ourselves/others/something bigger than ourselves.AI (including for emotional/psychological support)
Risk-taking (including anything from shoplifting to extreme sports)
Whether the behavior is a habit or an addiction, the underlying needs they are both trying to meet come down to feeling something good and/or avoiding feeling something bad. For example, both addictions and habits can be used to get social connection or to get a break from stress.
But there are three things that fundamentally distinguish an addiction from a bad habit:
The nature of the underlying need.
The degree of dependence on the behavior to meet it.
The degree of choice we feel about how or whether we do the behavior.
What Makes Something a “Bad” Habit?
When a behavior is simply a habit, it is something we do without thinking while fundamentally still having choice around whether we do it or not. It meets a need to feel good or get away from feeling something bad, but we don’t depend on it mentally, emotionally, or physically to meet that need.
Maybe you always enjoy a drink or two to unwind on Friday nights when you’re out to dinner with your partner. It could be that you usually eat an extra slice of pizza even when you’re full because the taste makes you happy, or even because it keeps you from feeling sadness or frustration. You go for runs every evening to burn off steam or mindlessly swipe on Tinder to feel less alone.
But when these things are habits, you know that you’re able to unwind, feel happy, blow off steam, or feel connected without doing those specific things. You tend to do them regularly and automatically, but you also feel that you have a variety of options for feeling something good or getting away from bad feelings. And you generally feel free to choose to do something different (even if you prefer what you usually do).
Another key element that distinguishes a habit from an addiction is that the underlying need a habit is trying to meet is usually not existential. It’s more about generally wanting to feel something good in a given moment or to avoid something that doesn’t feel so great, not about depending on the behavior to cope with the long-term impacts of trauma or intense psychological or physical pain. So when the option you might more habitually turn to in order to feel better is not available to you, you don’t go into a state of overwhelm, panic, or depression.
When you need to cut out your weekend drinks because you’re not making as much money, you don’t start to feel intense social anxiety around going out with your friends. When an injury from working out a bit too much means you need to stop until it recovers, you don’t start having panic attacks or fall into a deep depression as a result. While you might not be particularly excited about making the change, you can stop a habit without feeling too bad about it and adjust pretty quickly to its absence. Which is to say that when you stop, you don’t have psychological (let alone physical) withdrawals.
Because of the relative ease with which true habits can be shifted, the negative consequences don’t tend to pile up in the same way they do with addictions. We call something a “bad” habit specifically because we’re aware of the negative impacts a behavior might have on our physical or mental health or on our relationships. But the degree of bad stuff we’re willing to go through in order to continue engaging in a habit is far less than with an addiction because the need we’re trying to meet is not as intense.
My Truce with White Bread
This is exactly how I felt about white bread.
At the time I needed to make these dietary changes, I was probably eating more bread than my body was happy digesting, and doing so largely because it was convenient. I also freaking love bread. If given the choice, I would pick a fresh brioche roll for a sandwich over the gluten-free stuff any day.
But since I’ve had to pump the brakes, there have only been a few moments of very low-level frustration when presented with the choice of whether to bread or not to bread. I was able to make the switch in a matter of a couple of weeks, whether it was choosing a gluten-free option or skipping the traditional bread and tomato served at most restaurants here in Barcelona.
And when I do have bread once a week or so, I enjoy it for what it adds to my life and I’m fine to live without it the rest of the time. It’s worth it to me to be a bit inconvenienced if it means that my health will benefit.
But with sugar, it was the complete opposite.
What Makes Something an Addiction?
Where a habit is a repeated attempt to feel something good or avoid feeling something bad in a particular moment, an addiction is a psychological dependence on a compulsive behavior to protect against extreme emotional pain. This pain is usually related to experiences of harm and/or unmet core human needs that we continue to struggle with, whether because we are going through them now or because of unresolved past trauma.
This pain is so intensely overwhelming that a part of us is committed to us never feeling that way. Actively being in touch with this pain would stop us from functioning if it were allowed to be present all the time. If it’s not clear whether your behavior is an attempt to manage those feelings, I invite you to notice what happens when you wait for even five minutes between wanting to do the thing and actually doing it. You likely won’t directly feel that pain, but you will probably notice some kind of internal distress or blanking out, and likely a feeling of urgency around doing the thing.
Some of these painful internal experiences include:
Feeling alone in the world
Fear or terror
Anxiety
Depression
Feeling unworthy or not valuable
A baseline feeling of something being wrong with me
An addiction then forms as a way to meet the need to not experience these things, whether indirectly (by numbing them out or distracting from them) or more directly (by using the behavior to try to get the feeling I would want to have instead). Maybe I use Netflix to keep me from feeling the void inside of me, or I use ChatGPT to give me advice in a world where it feels unsafe to ask a human for help. Perhaps my drinking allows me to break through the walls that usually keep me trapped in a feeling of isolation, or smoking weed gets me away from the gnawing feeling of something being fundamentally wrong with me. Whatever our addiction is doing for us, the feeling we would have to experience if I weren’t doing those things is deeply overwhelming.
These internal experiences we’re trying to get away from can be the result of many different external events or circumstances, including one-time traumatic events (such as a death or divorce) and complex trauma (exposure to longer-term traumatic environments, including emotional and/or physical neglect and abuse, such as absent caregivers, lack of food/nutrition, lack of support/skills in managing emotions and relationships, etc.).
But it is not just these external factors alone that lead to the chronically overwhelming internal states that we cope with through addiction. It is the lack of support in navigating, coping with, and making sense of them that leaves us alone to figure out what to do with them. Without that support, the overwhelming experience lingers on as an eternal threat to our system that we have to keep at bay to be able to function. And any unmet needs desperately continue to seek to be met, often by any means necessary, including using behaviors that end up becoming addictions.
This also leads to there usually being significantly more negative consequences that we are willing to tolerate while continuing to engage in an addiction when compared to a habit. The more intense the experience we’re trying to cope with via our behavior, the more bad stuff we’re willing to put up with without making any real change - whether the bad stuff is more immediate (like losing a job or fighting with our partner) or long-term (like increasing our risk for lung cancer or damaging our cardiovascular health).
But don’t we always have a choice about our behavior?
While we could argue that on some absolute level we technically always have a choice about what we could do to meet the underlying need of the addiction (and therefore avoid the behavior’s negative consequences), that is not the reality of what it feels like.
When whatever our addiction is protecting us from experiencing is so extreme, the idea of not doing the thing doesn’t actually feel like an option (and some would say that it literally isn’t). The behavior is experienced as compulsive. For fear that we would catch even a glimpse of what our addiction is protecting us from, our system doesn’t allow us to have any awareness of the space between the impulse to do the thing and the action of following through on it. When that space can’t be perceived, there is essentially no conscious ability to make a choice.
Because the addiction is doing something so incredibly important for our system, we usually develop complementary behaviors that help to protect the addiction from being challenged or interfered with. These include:
Lying
Denial
Sneaking around
Hiding the behavior
Minimizing
And it is these ways of protecting our addiction that can often make it even harder to recognize that we have an addiction in the first place.
But what if nothing bad happened to me?
When I first bring up addiction as an attempt to meet the existential need of coping with deep pain, there are many people who struggle to believe it. They often say something like, “There can’t be anything that bad that I’m protecting myself from feeling or any deep needs that weren’t met… My life has been fine! That’s why I don’t understand why I can’t just stop. I think I’m just broken.”
What I say in return is something along the lines of, “If the thing you’re doing is messing with your life in real ways and you’re not making a change, that must mean there is something worse than the bad things you’re experiencing as a result of this behavior. What you would have to feel, face, or deal with by stopping must be worse. And that had to have come from somewhere.”
If it were true that there was nothing so bad, then we would stop. Because the negative consequences of what we’re doing wouldn’t be worth continuing to do it. And the degree of negative consequences we are willing to live with while continuing to engage in a behavior tells us something about the degree of intensity of whatever it is we’re protecting ourselves from or of the needs we’re trying to meet.
But since the whole point of the behavior is to keep the pain and the needs at bay, that also often means keeping us from fully knowing what it is that we are protecting ourselves from. This then also keeps us from seeing that there is always a reason why our addictive behaviors are actually trying to take care of us.
So many of us were never made aware of what we all actually need to develop into truly resilient people with solid self-esteem and trust in ourselves. So in the absence of acute, obvious traumatic events (and honestly, even with them), it can be really easy to minimize the pain of our unmet needs or the harm done to us. That’s why in addition to understanding the impact of traumatic events on our lives, it’s also crucial to have an understanding of complex trauma and how it affects us. Complex trauma is the experience of harm or unmet needs over a longer period of time, which can also include acute traumatic events but can happen even without them.
But aren’t certain things just addictive, even without the trauma?
The nuance here is that substances and behaviors do change our physiology, which can create a positive feedback loop of dependence on the behavior and resistance to stopping it. A behavior that started out as trying to feel good or less bad can, through the ways that it impacts our bodies and minds, end up multiplying the discomfort and pain that can happen when we try to stop doing it. This includes the pain of physical withdrawals when we become chemically dependent on a substance.
As we continue a behavior, it can also start to create its own negative consequences that we then use the same (or another) behavior to try to cope with. For example, a hangover from partying too much the night before might lead to a little hair of the dog the next morning. Or the lack of sleep from late-night Netflix binges might lead to relying on coffee and cigarettes to get through the next day. This is one of the key places where a habit can start to transition or lead to an addiction.
However, what I find over and over again is that the reason why certain addictive substances or behaviors are appealing to us to begin with, let alone why we’re willing to tolerate their negative consequences over significant periods of time, is because they finally give us the relief from the pain or meet the underlying need that our system has always had. It’s like finding the right puzzle piece for a hole that we may not have ever consciously realized we have.
The best example that I have seen too many times to count is young people becoming addicted to painkillers after a surgery. There are plenty of kids who are totally fine coming off the meds once they are healed enough to do so. But over and over again, I see that the people who struggled to come off of these meds found that they not only offered relief from physical pain, but they finally got relief from an internal pain that was already there before the surgery. So while our bodies can inherently become physically dependent on opiates, it’s often a hesitance to give up the emotional relief these meds offer that multiplies the difficulty stopping them. In other words, the emotional withdrawals they would have to go through by trying to stop the meds make the physical withdrawals even less worth going through.
But what about physical dependence?
Like opiates, there are many substances that we will develop a physical dependence on when used over long periods of time.
One aspect of physical dependence is the experience of physical withdrawals. When we try to stop using a substance we’re physically dependent on, we will experience (sometimes life-threatening) physical symptoms as we reduce how much we’re taking. This is especially true if stepping off of a medication or substance is not managed properly. These withdrawal symptoms can include headaches, nausea, sweating, shaking, cognitive impairment, and even death (in the case of alcohol and opiates).
Tolerance to the effects of a substance is another key aspect of physical dependence. Even if we’re taking medication as prescribed and strictly for the reason we were prescribed it, we might notice that we need more and more of the substance over time to get the same effects as we did when we started taking it.
The key misunderstanding when talking about physical dependence is to say that anyone who experiences withdrawals from a substance or develops a tolerance to it is addicted to it. That’s because physical dependence on a substance can happen both within and outside of an addiction.
Within an addiction, the physical dependence happens and is sustained because the substance is being used to manage emotional and psychological pain. The need to continue using becomes connected to both the emotional need the substance meets, but now also includes the need to avoid the very physical pain and discomfort of physical withdrawal. This can even more deeply entrench an addiction and simply make it more difficult to stop once we have decided that we might want to.
Outside of an addiction, we can be physically dependent on a substance without it meeting any deeper emotional or existential need. In that case, when we start to have negative effects from the medications, our threshold for the negative impacts of taking the substance that we will tolerate before at least attempting to stop them is usually much lower.
To go deeper on the previous example, let’s say that I’m on opiates for managing pain after a surgery, but the way I feel on them means that my close relationships are being damaged. When the time comes to come off of the meds, if they aren’t meeting any deep emotional needs for me, I would likely be willing to go through the physical withdrawals to make sure my relationships are maintained. But if those same pain meds happened to also be medicating deep feelings of loneliness or shame that I would have to feel again if I were to stop, I would likely be much less willing to step down and go through both the psychological and physical withdrawals.
(There is a more nuanced conversation here around long-term pain management that is incredibly important, but too big for this blog post. In those cases, this sense of choice around balancing pain management and the negative effects of the medications we might use becomes complex in a unique way.)
But my life isn’t falling apart, so it can’t be an addiction, right?
While the intensity of the negative external consequences of a behavior can be one indicator of an addiction’s overall severity, it isn’t the only measure. The true severity of an addiction is measured the intensity of negative internal and/or external consequences that a person sustains without being able to stop.
We usually paint the picture of someone in the throes of a “severe” addiction as someone who has faced more obvious negative external consequences as a result of their behavior. They’ve lost their job, irrevocably damaged their relationships, and maybe even ended up penniless.
And while all of those externally recognizable things do in fact indicate a severe addiction, it is also true that the person who shows up to work every day, seems to have it all together, and still calls everyone on their birthdays can be in the grips of an internal hell, the severity of which no one in their lives might be able to imagine.
These internal consequences, including the feelings of being trapped and out of control, can be just as damaging as the external consequences.
While there is no objective way to measure and compare the severity of addictions between people, one subjective measure is to ask ourselves: What degree of pain and suffering, whether internal or external, we are willing to endure as a result of our behavior while continuing to engage in it? The more severe the negative consequences we will tolerate, whether internal or external, the more severe the addiction (and the more severe the pain it’s protecting us from).
My Wake-Up Call
Even before the hormone issues snuck up on me, I was already reckoning with my relationship to sugar.
It was 2 in the morning when I found myself standing by the sink in my street-lamp-lit kitchen with a spoon in one hand, the yellow plastic Cacaolat mix container in the other, and a mouth full of sugary chocolate powder. As I tried not to inhale it before it dissolved and flooded my system with sweet relief, I kept an ear out for any sign that someone was headed to the kitchen, ready to hide the evidence if need be.
I wish I could say that this was the exact moment I fully realized that something was very wrong. And that this was my last secret middle-of-the-night sugar fix.
As you can probably guess: I didn’t. And it wasn’t.
For better or for worse, it took a bit more time (and more than a few more furtive spoonfuls of Cacaolat) to put all the pieces together. But this moment and too many others like it served as a giant hint that something was off. Not only was I driven to this level of cover-of-night desperation to get a sugar fix… I was decidedly hiding it.
It wasn’t until I couldn’t stop with the sugar after learning that it was a (if not the) culprit behind my hormone issues that I truly accepted that this was more than just a bad habit. When I added my more recent failed attempts to cut back on sugar to the many, many (many, many, many) other failed attempts over the years, I could no longer pretend that this wasn’t as “real” of an addiction as any other.
I was psychologically and emotionally dependent on sugar to meet a deeper existential need and felt no ability to choose whether or not to use it.
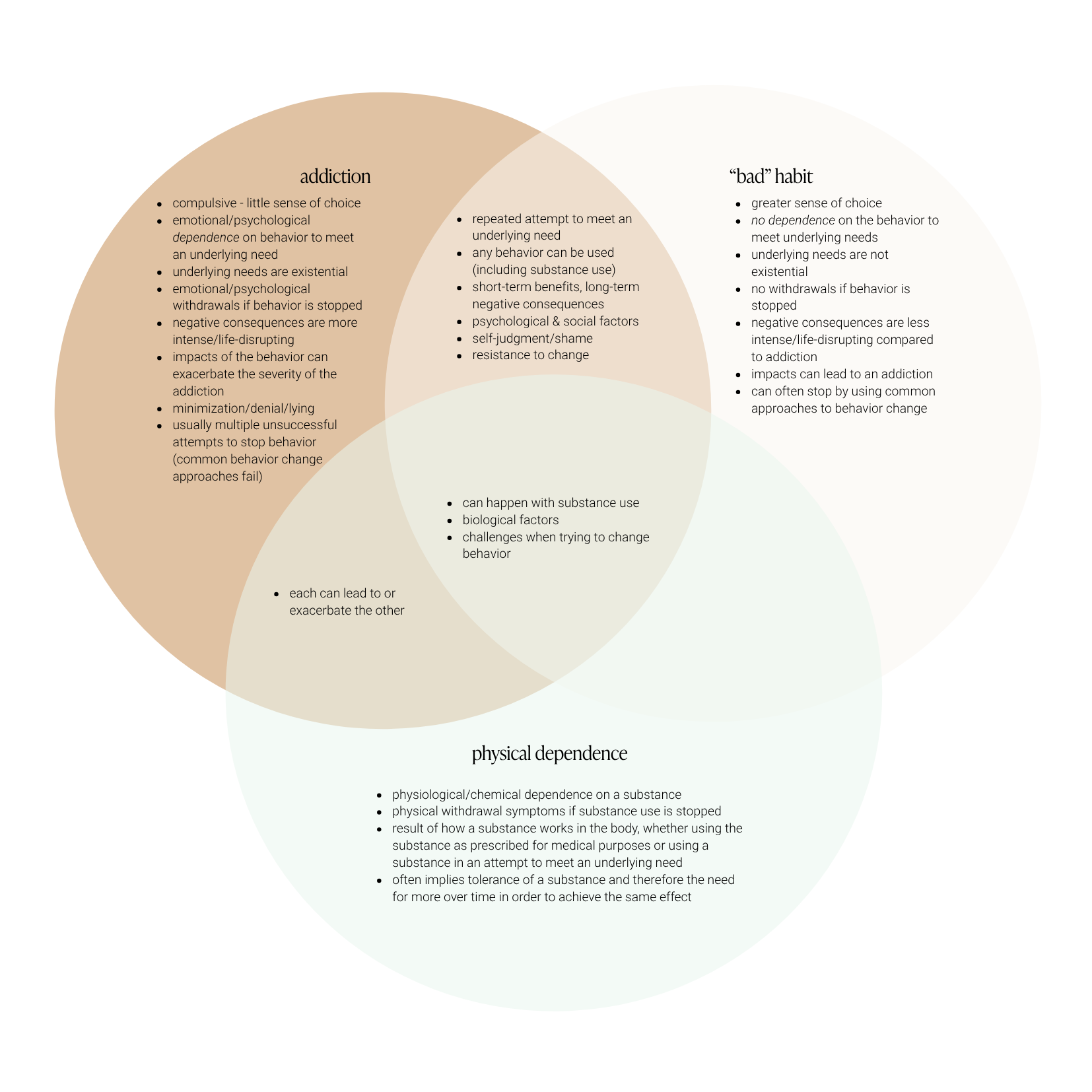
The Intersection: Addictions, Habits, & Physical Dependence
As we try to understand what is going on for us, it can be helpful to zoom out and to see how addictions, habits, and physical dependence intersect. While there is no obvious line we cross from one to the other, this kind of visual can help us to recognize where our behavior lies on the spectrum from habit to addiction, as well as where it might dip into physical dependence. From there, we can start to get clarity about how to move forward.
Why Does it Matter?
But why does it matter whether we call something an addiction or a bad habit?
Because when the time comes that we want to make a change, knowing whether we are dealing with a habit or addiction is the key to knowing what we need to do and what to expect from the process. The way we deal with a bad habit is simply not the same as what is needed to loosen the grip of an addiction.
We usually seek help with a behavior in one of two circumstances:
The negative consequences outweigh the benefits - this includes desires to “get healthy,” which is another way of saying the same thing
It stops “working” - the behavior is no longer helping in the way it used to
When we reach this point with a habit, traditional behavioral approaches can work relatively well. We can substitute the behavior for something else, finding other ways to feel good or to manage a bad feeling. We might also look a bit deeper into what makes it appealing to us to use certain behaviors that don’t always take into account our long-term wellbeing. We might find that we’re just simply repeating what was modeled for us and we weren’t fully aware of the long-term-healthier alternatives. Or we might find some issues around self-worth or self-doubt that we need to address in order to be willing to change the habit.
Often it is when these kinds of top-down approaches don’t work that we are forced to recognize that we might be dealing with an addiction after all. Behavioral change approaches or mindset changes will not by themselves offer any long-term relief for an addiction, usually leading to a lot of frustration for those who try these approaches. Especially for those of us who don’t want to believe that what we might be dealing with is actually an addiction.
And while we might need to do some top-down damage control and harm reduction in order to initially stabilize our addiction, that is only a preliminary step. If the benefit of the behavior was to stave off intensely overwhelming internal experiences, then the longer-term work of addiction recovery will inevitably take us into healing those tender spots we’ve been protecting ourselves from. That is a much more delicate, though deeply rewarding, path. And often one that takes a fair bit longer than the process of breaking a habit.
Please note: If you are dealing with physical dependence on a substance and wanting to stop using, please seek appropriate medical support before making any changes.
A Shortcut: The “Take It or Leave It” Test
As I was working on this article, I stumbled upon an Instagram story from fellow therapist Brian Costello with a familiar reflection about discerning whether something is a bad habit or something more. The key is that when something is just a habit, you can genuinely “take it or leave it,” where the “leaving it” is genuinely just as easy as the “taking it.”
When you really ask yourself whether that’s the case, it starts to become clearer when what you might have thought was a habit has crossed into addiction territory.
I had heard versions of this reflection many times before, but in this moment it hit exactly what I was trying to communicate about my own process: It was when I knew in my bones that leaving the thing was infinitely harder than taking it that my denial finally evaporated.
But while my story ends with recognizing an addiction that I was previously in denial of, I want to be clear that this isn’t the way it ends for many people.
No, we are not all addicted to something.
Sometimes we regularly do things that might not have the greatest long-term consequences, but that we are genuinely completely in control of and still choose to do anyway because they meet a short-term desire or need.
Given that, our work here is to be as honest as possible with ourselves in the face of the question: Is the leaving just as easy as the taking? Or do you only wish that were the case?
Want to explore working together?
If you want to make a change in your behavior or you’re struggling with the impacts of someone else’s behavior (whether it’s an addiction or a habit), you’re welcome to schedule a free 20-minute discovery call to see if we’d be a good fit.
Want to stay in touch?
Join my Substack to stay updated with new posts, courses, events, and availability for individual, couples, and group sessions.
References
Books:
In the Realm of the Hungry Ghosts by Gabor Maté
Internal Family Systems Therapy for Addictions by Cece Sykes (written for therapists)
Additional Resources:
Podcasts featuring Cece Sykes